How We Help Medicaid & Long-Term Services and Supports
NCQA
JUNE 27, 2023
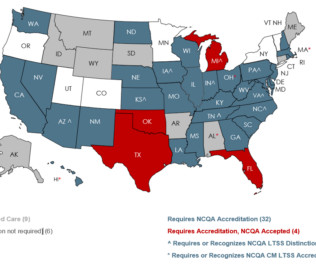
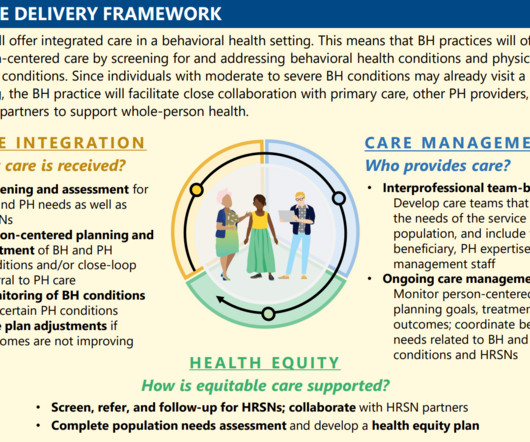
More states are contracting with managed care organizations (MCO) to provide Medicaid long-term services and supports (LTSS). How do we know if MCOs are delivering equitable, high-quality care to people receiving LTSS? The post How We Help Medicaid & Long-Term Services and Supports appeared first on NCQA.
















Let's personalize your content